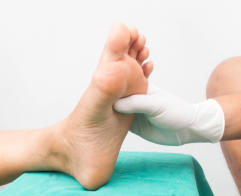
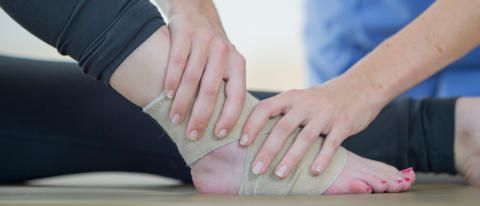
Many people are surprised to learn the wide variety of services
provided by a podiatrist. Dr. May is trained and experienced in
the latest techniques and is prepared to provide you with the
most comfortable treatment possible.
Why Choose Illinois Foot & Ankle Center?
We put our patients first. Dr. May is committed to understanding the
needs of each patient and explaining the treatment options available.

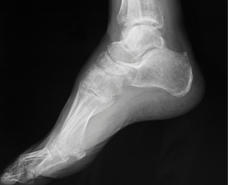
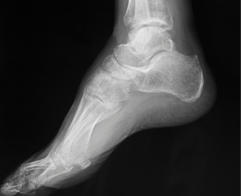
Our on-site digital x-ray means a diagnosis can usually be made on your
first visit, without extra visits to the hospital or imaging center.

We offer the latest in cutting edge technology to provide you with the
best treatment options possible to get you back on your feet sooner.

While the course of treatment may vary from patient to patient, many of the conditions treated are very
similar. There is, however, a very wide variety of foot and ankle conditions that Dr. May is highly trained
to treat. Below are some of the more common ones and some information on each of them.
Common Conditions Treated by Dr. May


2024 Illinois Foot & Ankle Center, SC.
All rights reserved.
If you are experiencing a medical emergency please dial 911 or visit the nearest urgent
care or emergency department.
Sitemap
Section 1557 Notice of Nondiscrimination























Achilles Tendon Disorders
The Achilles tendon is the strongest tendon in the human body. Its purpose is to connect the lower leg muscles and calf to the heel of the foot.
This tendon is responsible for facilitating all types of movement, like walking and running. Since this tendon provides an enormous amount of
mobility to an individual, any injuries inflicted to this tissue should be immediately brought up with a physician to prevent further damage.
The most common injuries that can trouble the Achilles tendon are tendon ruptures and Achilles tendinitis. Achilles tendinitis is the milder of
the two injuries and can be recognized by the following symptoms: inflammation, dull to severe pain, an increased flow of blood to the tendon,
thickening of the tendon, and slower movement time. Tendinitis can be treated via several methods and is often diagnosed by an MRI.
An Achilles tendon rupture is trickier to heal, and is by far the most painful injury. It is caused by the tendon ripping or completely snapping.
The results are immediate and absolutely devastating, and will render the patient immobile. If a rupture or tear occurs, operative and non-
operative methods are available. Once the treatment begins, depending on the severity of the injury, recovery time for these types of issues can
take up to a year.
Simple preventative measures can be taken as a means to avoid both injuries. Prior to any movement, taking a few minutes to stretch out the
tendon is a great way to stimulate the tissue. Calf raises, squats, leg curls, leg extensions, leg raises, lunges, and leg presses are all suggested
ways to help strengthen the lower legs and promote Achilles tendon health.
Many problems arise among athletes and people who overexert themselves while exercising or who do not properly warm up before beginning
an activity. Proper, comfortable shoes that fit correctly can also decrease tendon injuries. Some professionals also suggest that when exercising,
you should make sure that the floor you are on is cushioned or has a mat, as this will relieve pressure on the heels. As always, a healthy diet will
also increase tendon health.
It is very important to seek out a podiatrist if you believe you have an injury in the Achilles region, because further damage could result in severe
complications that would make being mobile difficult, if not impossible.

Ankle Pain
Pain experienced in the ankle can be caused by a multitude of conditions. While the most common cause is an ankle sprain, other possible
problems can include arthritis, gout, ankle instability, ankle fracture, nerve compression, or tendinitis. In more serious cases, ankle pain can be
a sign of improper alignment of the foot or an infection.
Ankle pain can often be accompanied by symptoms such as redness, swelling, stiffness and warm in the affected area. Pain can be described
differently depending on the condition; short, stabbing pain and a dull ache are some examples. If such symptoms are persistent and do not
improve after time, be sure to schedule an appointment with your local podiatrist.
Depending on the condition behind your ankle pain, different treatments may be prescribed by your podiatrist. For ankle sprains, the first step
in treatment involves rest, ice, elevation, and compression. Be sure to avoid placing pressure on the ankle, use an ice pack several times a day,
and use a compression bandage and elevation to reduce swelling. Other more serious conditions may require the assistance of certain drugs and
medications such as non-steroidal anti-inflammatory drugs (NSAIDs), physical therapy, or even cortisone injections.
Consult with your foot and ankle doctor to best determine the cause of your ankle pain and the appropriate treatment. Depending on the
severity of your ankle pain and the condition behind it, recovery from ankle pain may take some time.

Ankle Sprains
Ankle sprains can be serious and should be given immediate attention and care, despite not being as severe as a broken ankle. An ankle sprain
can lead to a significant amount of pain, as well as limited mobility. They are often characterized by swelling and discoloration of the skin, which
occurs when the ligaments are stretched beyond their limits.
The simple act of walking can sometimes cause a sprain, which makes them a very common injury for anyone. They occur when the ankle twists
in an awkward way or rolls over itself, causing a pop or snap in the tendons around the ankle. Some people are more at risk than others,
including athletes who continually push their bodies to the limits and also people who have previously suffered accidents to the feet, ankles, or
lower legs.
If you believe you have an ankle sprain, it is important to consult with your podiatrist right away. Ankle sprains can turn into severe injuries that
may require hospitalization. If the ankle ligaments or muscles are damaged from a tear or rip, the sprain may be severe enough to warrant going
to the hospital and possibly having surgery done. Even after surgery the recovery process can be long, often involving rehabilitation sessions with
a podiatrist to get your ankle back to full strength and health.
The severity of your sprain may become apparent if you are unable to stand or walk, if non-stop pain is occurring over a prolonged period of time,
if swelling is much more severe than initially present, or if you start to experience tingling or numbness. These signs may show that your ankle
sprain might actually be a broken ankle, which requires immediate medical attention.
While not completely avoidable, ankle sprains can be curbed with some preventative treatment measures. These include wearing appropriate
fitting shoes that not only provide a comfortable fit, but also ankle support. It is also recommended to stretch before doing any kind of physical
activity, as this will help lower your body’s chance for an injury.

Arthritic Foot and Ankle Care
During your lifetime, you will probably walk about 75,000 miles, which is quite a lot of stress to put on your feet. As you get older, the 26 bones
and 30 joints in your foot will lose flexibility and elasticity, and your foot’s natural shock absorbers will wear down too. Having arthritis in
addition to life’s wear and tear only makes matters worse; the joints will become distorted and inflamed, making arthritic foot care an important
thing to consider for your overall health.
When dealing with arthritis, having additional foot complications—such as bunions, hammertoes, or neuromas—may be a serious detriment. To
avoid these, buying well-fitting shoes with a lower heel and good support is a must. Having shoes with good arch support is highly recommended.
Aside from getting good arch support, the shoes need to fit comfortably and properly as well. A good place to start is by leaving a finger width
between the back of the shoe and your foot to gauge proper size. It is also helpful to have a square or rounded toe box in the front to provide even
more comfort. Another thing to look for is a rubber sole that can provide a cushion and absorb shock as you walk. This adds flexibility to the ball
of your foot when you push off your heel to walk.
Exercise is another key aspect of arthritic foot care, as it not only strengthens and stretches the muscles and joints but helps prevent further
injury and pain as well. Certain non-steroid, non-inflammatory drugs or topical medicines may be recommended by your podiatrist to help ease
arthritic pain. Be sure to visit your podiatrist to determine what method of care is best for you.

Athlete’s Foot (Foot Fungus)
Athlete’s foot is an extremely contagious infection caused by a fungus that results in itching, burning, dry, and flaking feet. The fungus that causes
Athlete’s foot is known as tinea pedis and thrives in moist, dark areas such as shower floors, gyms, socks and shoes, commons areas, public
changing areas, bathrooms, dormitory style houses, locker rooms, and public swimming pools. Athlete’s foot is difficult to treat as well because of
the highly contagious and recurrent nature of the fungus.
Athlete’s foot is spread by direct contact with an infected body part, contaminated clothing, or by touching other objects and body parts that have
been exposed to the fungus. Because the feet are an ideal place for tinea to grow, thrive, and spread, this is the most commonly affected area, but
it is known to grow in other areas.
The most commonly infected body parts are the hands, groin, and scalp, as well as obviously the feet. Around 70% of the population suffer from
tinea infections at some point in their lives, however not all of these cases are Athlete’s foot. Just like any other ailment, some people are more
likely to get it than others; such as people with a history of tinea infections or other skin infections, both recurring and non-recurring ones. On top
of this, the extent to which a person experiences regrowth and recurrent tinea infections varies from person to person.
Sometimes people will not even know that have Athlete’s foot because of a lack of symptoms. However, most people experience mild to moderate
flaking, itching, redness, and burning. Some of the more severe symptoms include cracking and bleeding skin, intense itching and burning, pain
while walking or standing, and even blistering.
Because of the recurring nature of tinea fungus and the Athlete’s foot it causes, the best way to treat this condition is with prevention. While it is
hard to completely avoid, you can take some preventative measures such as wearing flip flops or sandals in locker rooms and public showers to
reduce contact with the floor. It is important to keep the feet clean and dry, which will allow them to air out and breathe. If you suspect you have
Athlete’s foot, immediately visit your local podiatrist to determine what treatment is best for you.

Bunions
A bunion is an enlargement of boney growth or swollen tissue typically located at the base joint of the big toe. The condition is caused by the
shifting of the bones in the big toe inward, toward the other toes of the foot. The area around the base of the big toe may become inflamed, red,
and painful.
Genetic factors are important in the formation of bunions – people who get bunions are usually genetically predisposed to this bone
displacement and may cause its onset by wearing ill-fitting shoes or by running or walking in a way that causes stress to the feet. Another
common cause for bunions is wearing high heeled shoes. The weight of the body in these shoes pushes the toes into an unnatural position,
possibly causing bone displacement.
A podiatrist who specializes in foot structure and biomechanics can quickly diagnose bunions. Bunions must be distinguished from gout or
arthritic conditions, so blood tests may be necessary. The podiatrist may order a radiological exam to provide an image of the bone structure. If
the x-ray demonstrates an enlargement of the joint near the base of the toe and a shifting toward the smaller toes, this is indicative of a bunion.
Wearing wider shoes can remove the pressure on the bunion and reduce pain. High heeled shoes should be eliminated for a period of time as
this type of shoe generally pushes the big toe outward toward the smaller toes. This may be enough to eliminate the pain associated with
bunions; however, if pain persists, anti-inflammatory drugs may be prescribed. Severe pain may require an injection of steroids near the
bunion.
Orthotics for shoes may be prescribed which, by altering the pressure on the foot, can be helpful in reducing pain. These do not correct the
problem, but by eliminating the pain, they can provide relief.
For cases that do not respond to these methods of treatment, surgery can be done to reposition the toe. A surgeon may do this by either taking
out a section of bone or by rearranging the ligaments and tendons in the toe to help keep it properly aligned. It may be necessary even after
surgery to wear more comfortable shoes that do not put pressure on the toe as the big toe can easily move back to its orientation toward the
smaller toes.

Corns
Corns are thickened areas on the skin’s surface, to the point of being irritating and sometimes painful. Commonly found on the feet, corns are
circular or cone-shaped and develop where there are areas of pressure or friction, such as on the little toe when it rubs up against shoes or on
the ball of your foot.
Corns are often confused with a callus, but there is a difference between them. Corns can be raised bumps that are painful to the touch. They
consist of a rough, thick area of skin that may be dry or waxy. Corns tend to be surrounded by skin that is inflamed, and are usually much
smaller than calluses.
The best treatment for a corn varies from person to person and is best determined by a podiatrist. Certain topical over-the-counter products
may be suggested, or a more serious treatment may be prescribed. Diabetics should consult with a podiatrist immediately if they have
developed a corn, as small wounds such as corns can develop into more serious conditions.
Orthotic inserts, which are fitted by a podiatrist, may also help with treating corns. Inserts fit right into the shoes and adjust the way the feet fit
into the shoes, thus fixing the way one walks. Proper-fitting orthotics can help reduce friction, which can in turn help reduce corn formation
and exacerbation.
Surgery can be used to treat corns. Corn surgery actually deals with the underlying issue that causes corns. During surgery, the bone is shaved
and any abnormalities are corrected, thus reducing the amount of friction that occurs during walking.
To prevent corns, the first step is reducing friction. Always wear shoes that fit well and don’t rub the feet. Wearing cushioned insoles in your
shoes can also reduce friction. While there are many ways to prevent corns, it is best to consult a podiatrist with any questions you may have.

Custom Orthotics
Orthotics are shoe inserts that are meant to correct an irregular walking gait or provide cushioning to the feet. Orthotics come in a variety of
different models and sizes, including over-the-counter and customizable variants. Customizable orthotics can be shaped and contoured to fit
inside a specific shoe and are typically prescribed through a podiatrist who specializes in customized footwear and orthotics design and
management.
Customized footwear and orthotics design and management. Orthotics are beneficial because they can help prevent injuries from occurring
and provide cushioning to keep pain levels down to a minimum. They also allow for the correct positioning of the feet. Orthotics can act as
shock absorbers to help remove pressure from the foot and ankle. Therefore, orthotics can make bodily movements, such as walking and
running, become more comfortable as well as help prevent the development of certain foot conditions.
Orthotics alleviate pain and make the foot more comfortable by slightly altering the angle at which the foot strikes the ground surface,
therefore controlling the movement of the foot and ankle. Orthotics come in different variants and can be made of various materials. To
determine what type of orthotic is most suited to your feet and your needs, it is best to consult your podiatrist. He or she will be able to
recommend a type of orthotic that can help improve your foot function or prescribe a custom orthotic to best fit your feet.

Diabetic Foot Care
Diabetes affects millions of people every year. Blood vessels located all over the body are damaged due to diabetes—even the blood vessels of
the feet. Neuropathy, or nerve damage, can result from slower blood flow in the legs and feet. In diabetic patients neuropathy is very important
to monitor, as diabetics are at risk for developing ulcers.
Always washing and thoroughly drying the feet are pertinent parts of diabetic foot care. There should be a focus on cleaning between the toes.
Even if no pain is felt, the entire foot should be examined for redness and sores. Neuropathy can often mask the pain of sores and ulcers, and
cause these conditions to be overlooked. Use a mirror to examine the underside of your feet if needed. It is recommended that diabetics wear
will-fitting socks.
Patients with diabetes should have their doctor monitor their blood levels because blood sugar levels play a huge role in diabetic care.
Monitoring these levels on a regular basis is highly advised. It is very important to keep your blood sugar levels in the normal range, which can
be determined by your physician. There are medications that a physician may prescribe to help with neuropathy of the diabetic patient. It is
also advisable to visit a podiatrist if the diabetic patient is experiencing any conditions involving the feet such as ingrown toenails, which in
more severe cases can cause infection.
Diabetic foot care at home is possible if a patient is provided with instructions from their physician. Patients can cure dry heels with creams or
ointments. If trying to remove a callus with a tool, practice caution as severe diabetics may not be able to feel pain. Improper removal may
cause a wound to develop.
Diabetic feet must be inspected on a daily basis. Set up regular visits with your podiatrist since proper diabetic foot care is necessary. If you
suspect that you have a wound, notify your doctor immediately. Gangrene is a serious problem for diabetics and can lead to sepsis and
amputation in its worst cases. Early treatment and daily inspection of diabetic feet are keys to staying healthy.
Learn about Diabetic Wound Care

Flat Feet
Flat feet is a condition in which the arch of the foot is depressed, generally making the sole of the foot completely or almost completely stay in
contact with the ground. About 20-30% of the population generally has flat feet because their arch never formed during growth.
Having flat feet can sometimes make it difficult to walk due to the stress it places on the ankles. The general alignment of your legs is thrown
off because the ankles move more inward which can cause some major discomfort. This also has a big effect on the knees as many people that
have flat feet often have arthritis in that area. However, in many cases, having flat feet do not cause any pain and it should not be a cause for
concern in that case.
For those who run, there are specific shoes to help realign the ankles with a lot more support and less pronation. The weight shifting in this
activity is very quick, so that's why it's important to know if you have flat feet early on in your life, in case of injury down the road.
Symptoms of flat feet can include: pain around the heel or arch area, trouble standing on the tip toe, swelling around the inside of the ankle,
flat look to one or both feet, and having your shoes feel uneven when worn. A major cause of flat feet is never having developed an arch on your
foot. Overtime, a lot of stress and trauma to the foot can actually weaken the posterior tibial tendon that runs around the inside of the ankle.
This is the reason why some people with flat feet have pain around that particular area.
There are a number of ways to help treat flat feet. One way is going barefoot. Studies have shown that those that grew up going barefoot or
wearing less closed-toe shoes actually have more of an arch because the general strength and fullness of the arch increased. Also, those with flat
feet have a weaker Achilles tendon, and exercise to the area will help stretch the area. In a lot of cases, there are great shoe inserts provided by
podiatrists to provide ankle support as well as reduce the symptoms that go along with severe flat feet. For those that suffer severe pain in that
area, tendon surgery is an option to help with any posterior tibial tears.

Foot Pain
The feet, being the foundation of the body, carry all of the body’s weight and are therefore prone to experiencing pain and discomfort. If you
are experiencing foot pain, it is important to determine where in the foot you are experiencing this pain to help discover the cause of it. While
pain can be experienced virtually anywhere in the foot, the most common sites of foot pain are in the heel and ankle.
Heel pain can be due to a multitude of conditions including plantar fasciitis, Achilles tendinitis, and heel spurs. Pain experienced in the ankle
can be a sign of an ankle sprain, arthritis, gout, ankle instability, ankle fracture, or nerve compression. In more serious cases, pain the foot can
be a sign of improper alignment or an infection.
Foot pain can be accompanied by symptoms including redness, swelling, stiffness and warmth in the affected area. Whether the pain can be
described as sharp or dull depends on the foot condition behind it. It is important to visit your local podiatrist if your foot pain and its
accompanying symptoms persist and do not improve over time.
Depending on the location and condition of your foot pain, your podiatrist may prescribe certain treatments. These treatments can include but
are not limited to prescription or over-the-counter drugs and medications, certain medications, laser treatment, shockwave therapy, cortisone
injections, or surgery.
If you are experiencing persistent foot pain, it is important to consult with your foot and ankle doctor to determine the cause and location. He
or she will then prescribe the best treatment for you. While milder cases of foot pain may respond well to rest and at-home treatments, more
serious cases may take some time to fully recover.

Foot Surgery
In most cases, foot surgery is often chosen as the last-available option for conditions that have otherwise been unsuccessfully treated. Surgery
may be necessary for several reasons, including the removal of foot deformities (e.g. bone spurs or bunions), arthritis problems, reconstruction
due to injury, and congenital malformations (e.g. club foot or flat feet). Regardless of one’s age, foot surgery may be the only successful option
for treatment for certain conditions.
The type of surgery one undergoes depends on the type of foot condition the patient has. For the removal of a growth, such as a bunion, a
bunionectomy is necessary. If the bones in the feet need to be realigned or fused together, a surgical fusion of the foot is needed. For pain or
nerve issues, a patient may require surgery in which the tissues surrounding the painful nerve are removed. Initially, less invasive treatments
are generally attempted; surgery is often the last measure taken if other treatments are unsuccessful.
While in many cases surgery is often deemed as the final resort, choosing surgery comes with certain benefits. The associated pain experienced
in relation to the particular condition is often relieved with surgery, allowing patients to resume daily activities. The greatest benefit, however, is
that surgery generally eliminates the problem immediately.
Podiatry history has shown that foot treatments continue to evolve over time. As technology vastly improves, so will the various techniques in
foot surgery, which already require smaller and smaller incisions with the use of better and more efficient tools. Thanks to such innovations,
surgery is no longer as invasive as it was in the past, allowing for much faster and easier recoveries.

Fungal Toenails
Toenail fungus is a condition that many people develop and suffer from. Toenail fungus often results in the discoloration and thickening of the
toenail, which can cause embarrassment for many people. The condition begins as a small white or yellow growth beneath the tip of the nail
and at its worse can develop into the nail’s deterioration.
Thick, ragged, and distorted nails lacking shine are a sign of toenail fungus. The color of the affected nail tends to be darker because of debris
buildup underneath the nail. Toenail fungus is more likely to develop for people who wear socks and shoes that do not allow decent ventilation
of the feet. Public showers, gyms, and swimming pools are breeding grounds for toenail fungus, as their damp and humid environments allow
for the growth of bacteria.
Patients should visit their local podiatrist if they suspect they have toenail fungus because in its more severe stages, toenail fungus can become
very painful. Other infections can develop from toenail fungus that can spread to other parts of the body. Upon examination for fungus, your
podiatrist may scrape your nails if he or she finds debris. This will be sent to a lab to determine what fungus is causing the condition.
Toenail fungus can also be treated with certain over-the-counter antifungal creams and ointments. To remove pressure from the nails, keep
them cut at a short length. Oral antifungal drugs, medicated nail cream, or medicated nail polish may also be prescribed by your podiatrist if
simpler treatments do not prove successful. In some cases, your podiatrist may also recommend laser treatment to eradicate toenail fungus.

Geriatric Foot Care
While proper foot care is important for everybody, senior citizens have the tendency to be more susceptible to certain conditions and should
therefore be well informed about problems that may arise and what they can do to properly avoid or treat them.
Some of the most common problems are foot ulcers, ingrown toenails, fallen arches, and fungal infection. A foot ulcer is an open sore on the foot
and can be a result of decreased sensation in the feet. An ingrown toenail is defined as when the nail grows into the side of the toe. Fallen arches
are indicated by the instep of the foot collapsing. A fungal infection is a condition that results in deformed and discolored toenails.
In order to avoid these conditions it is recommended that the feet be inspected by the patient on a regular basis. If these inspections are carried
out routinely, there is a good likelihood that problems can be identified before they become severe, or can even be avoided altogether. If any
abnormality is discovered, it is important that the individual consult a doctor for diagnosis and information on treatment options.
Proper foot hygiene is also important. Making sure that you always have clean, dry socks on can be a major deterrent to many different problems
including bacterial infections, foot odor, and certain types of fungus. Wet feet are a major cause of many of these problems. If your socks get wet,
it is important to change them. Walking around in wet socks may not only lead to various infections, but can irritate the skin and result in a
number of various complications. Clean, dry feet are less likely to be affected by fungal and other infections.
As people age, the fat present on your feet begins to deteriorate. The protective nature of this fat keeps the feet healthy by providing a barrier and
between your bones and the ground as well as giving the skin on the foot a certain amount of elasticity. This is one factor that causes elderly
people to develop some serious foot issues. Foot moisturizers can be helpful to avoid certain problems associated with this.
However, water-based moisturizers do not work as well for elderly people as they do for the young. Instead, it is more effective to use an
emollient instead. An emollient is effective because it binds the water in the foot, keeping it from becoming absorbed too readily which will result
in dry skin. They also have a special property called occlusion, which provides a layer of oil on the skin. This layer prevents the foot from drying
up and can be very effective in treating dry skin disorders. If you can keep the skin on your feet healthy, this will substantially reduce the
number of foot problems you will encounter in old age.
Proper footwear is another way to keep feet healthy. Shoes that fit well and provide proper support help prevent ingrown toenails and fallen
arches.
Certain medical conditions such as diabetes or poor blood circulation increase the risk for foot issues. For individuals with any of these
conditions it is extremely important to conduct regular foot inspections to make sure that there are no sores or infections present.

Hammertoe
Hammertoes are painful deformities that frequently form on the second, third, or fourth toe. The condition is often caused by an issue in foot
mechanics: the person’s particular gait or the manner in which they walk, or shoes that do not comfortably fit the deformity. Hammertoes can be
formed after wearing shoes that are too narrow or short for the foot or have excessively high heels. Shoes that are not properly sized will force the
toes into a bent position for long periods of time, causing the muscles to shorten and toes to bend into the deformity of a hammertoe.
Hammertoe can also be caused by complications from rheumatoid arthritis, osteoarthritis, trauma to the foot, heredity, or a cerebral vascular
accident. Pain and difficult mobility of the toes, deformities, calluses, and corns are all symptoms of a hammertoe.
Someone who suspects they have the symptoms of a hammertoe should consult with a physician—particularly a podiatrist. Podiatrists diagnose
and treat complications of the foot and ankle. If the podiatrist discovers that the affected toes are still flexible, treatment for the hammertoe may
simply involve exercise, physical therapy, and better-fitting shoes. Treatment for hammertoes typically involves controlling foot mechanics, such
as walking, through the use of customized orthotics.
For more serious cases in which the toes have become inflexible and rigid, surgery may be suggested. During the operation, the toe would receive
an incision to relieve pressure on the tendons. A re-alignment of the tendons may then be performed by removing small pieces of bone to
straighten the toe. In some cases, the insertion of pins is needed to keep the bones in the proper position as the toe heals. The patient is usually
allowed to return home on the same day as the surgery.
If surgery is performed to repair a hammertoe, following the postoperative directions of your doctor is pertinent. Directions may include several
stretches, picking up marbles with your toes, or attempting to crumple a towel placed flat against your feet. Wear shoes that have low heels and a
wide amount of toe space to maintain comfort. Closed shoes and high heels should be avoided. Shoes with laces allow the wearer to adjust how
fitted her or she may want the shoes to be and also allow for greater comfort. To provide adequate space for your toes, select shoes that have a
minimum of one-half-inch of space between the tip of your longest toe and the inside of the shoe. This will also relieve pressure on your toes and
prevent future hammertoes from forming. Other preventative measures that can be taken include going shopping for new shoes in the middle of
the day. Your feet are its smallest in the morning and swell as the day progresses; trying on and purchasing new shoes midday will give you the
most reliable size. Be sure to check that the shoes you purchase are both the same size. If possible, ask the store to stretch out the shoes at its
painful points to allow for optimum comfort.

Heel Pain
Have you ever gotten up from a chair or out of bed in the morning, and upon taking that first step, feel like your heel has stepped on a tack?
Many people experience a feeling of sharp pain which radiates into their arch from their heel and which does not allow them to put their heel on
the floor. Sometimes they need to sit back down, stand only on their toes and use the wall for balance. If you can take a few steps, it seems to go
away and lessens, allowing you then to resume your activity. Later, throughout your day and after a period of rest, it can happen again. If this
sounds familiar you may be suffering from your first attack of heel pain.
Heel pain is a debilitating condition that affects day to day activities. Running and walking both cause stress on the heel because the heel is the
part of the foot that hits the ground first. This means that the heel is taking on your entire weight. Diagnosis and treatments for heel pain can be
easily found through your podiatrist.
Plantar Fasciitis
One of the main causes of heel pain is a condition known as plantar fasciitis. The plantar fascia is a band of tissue that extends along the bottom
of the foot, from the toe to the bottom of the heel. A rip or tear in this ligament can cause inflammation of these tissues, resulting in heel pain.
People who do not wear proper fitting shoes are often at risk of developing problems such as plantar fasciitis. Unnecessary stress from ill-fitting
shoes, weight change, excessive running, and wearing non-supportive shoes on hard surfaces are all causes of plantar fasciitis.
Achilles Tendinitis
Achilles tendinitis is another cause of heel pain. Similar to plantar fasciitis, inflammation of the Achilles tendon will cause heel pain due to stress
fractures and muscle tearing. A lack of flexibility of the ankle and heel is an indicator of Achilles tendinitis. If left untreated, this condition can
lead to plantar fasciitis and cause even more pain on your heel.
Heel Spur
A third cause of heel pain is a heel spur. A heel spur occurs when the tissues of the plantar fascia undergo a great deal of stress, leading to a
separation of the ligament from the heel bone entirely. This results in a pointed fragment of bone on the ball of the foot, known as a heel spur.

Heel Spurs
Heel spurs are essentially a hook of bone that forms at the back of the foot, at the base of the ankle. Heel spurs are also described as a calcium
deposit that covers the tendons and ligaments of the ankle. Heel spurs cause extreme pain, and can prevent someone from walking or being
physically active at a normal level.
Heel spurs are more common than people expect them to be. They are most common in people age forty and over, although heel spurs can occur
in people younger than forty, and frequently affect athletes or people who are very physically active. Heel spurs are also common in those with
poor circulation and degenerative diseases. People who suffer from arthritis may suffer from heel spurs as well.
The symptoms of heel spurs are pain in the lower ankle, which increase when walking. Treatment of heel spurs can be treated many ways and
most often times is very effective. If someone suspects that they have heel spurs, they should contact their physician. Their physician will
recommend that they perform an x-ray on the patient's ankles. The physician may also perform a physical on the patient to ensure that there are
no underlying conditions, and of course if heel spurs are discovered a physician can recommend treatment options.
Orthopedic shoes are specially designed footwear for people who suffer with foot problems. Orthopedics offer a rubber sole, which cushions the
heel and adds comfort to those who suffer from heel spurs. Another simple way to help the pain of heel spurs is to elevate the ankle to diminish
the pain. When elevating the ankle, the blood is not focused on that area of the foot and can bring some relief. When all these options have been
attempted, and there is still no relief from heel spurs, or the heel spurs return, surgery can be the more dramatic and permanent way to rid
patient of heel spurs.
There are less conventional ways that are becoming more popular ways to treat heel spurs. One option would be to use a night splint which
reduces the pain caused from heel spurs if worn overnight. Other alternative treatment methods that can be used are ultrasound, or acupressure.
There are also other tolls that can be used are heel cups, heel seats, heel pads, arch supports, and insoles.
Exercise is also another powerful tool to help alleviate pain from heel spurs and can help in dealing with some of the symptoms, although
exercising incorrectly and forgetting to protect your feet can lead to further pain. It is important to remember the correct way to place the feet
when exercising so as to avoid making the problems worse, or creating problems. When exercising to alleviate heel spurs, exercising strengthens
muscles around the surrounding tissue around the ankle. Stretching will also keep the tendons around the ankle flexible.

Ingrown Toenails
An ingrown toenail is caused when a toenail grows sideways into the bed of the nail, causing pain and swelling. The nail can sometimes
exacerbate and become infected, creating serious drainage.
There are many risk factors that can predispose a person to this common condition. Cutting your nails too short, participating in sports,
diabetes, being overweight, or having a fungal infection of the toe can all cause an ingrown toenail. The condition can often be related to
genetics, as many people are genetically predisposed to ingrown nails. More often than not, the problem can arise from wearing ill-fitting
shoes or from shoes that keep the feet slightly damp.
To prevent ingrown toenails, allow your toenails to grow a little longer and avoid cutting them too short. If you do develop an ingrown nail,
soaking the toe in hot water will help prevent infection and lessen pain. You may want to add antibiotic soap or Epsom salts to the water,
which will provide further protection against infection.
There are many quick treatments available for ingrown toenails that can lessen pain and have you walking with comfort. If your pain is so
severe that it keeps you from everyday activities, however, a visit with your podiatrist is necessary.

Neuromas
Morton's Neuroma, also called Intermetatarsal Neuroma or Plantar Neuroma, is a condition that affects the nerves of the feet, usually the area
between the third and fourth toe. Neuroma refers to a benign growth that can occur in different parts of the body. Morton's Neuroma strictly
affects the feet. This condition causes the tissue around the nerves that lead to the toes to become thick, causing pain in the ball of the foot.
This condition can be caused by injury, pressure or irritation. Normally no lump will be felt, but instead burning pain in the ball of the foot that
will often be sensationalized in the toes will be experienced. Numbness and tingling may also occur. With the onset of this condition, a person
may feel pain when tight or narrow shoes are worn. As the condition worsens, the pain may persist for days, or even weeks.
Persistent foot pain should always be a concern. The foot should be examined by a podiatrist if pain persists longer than a few days with no relief
from changing shoes, or relieving stress from the foot. The earlier the foot is examined and treated, the less chance there will be for needing
surgical treatment.
There are some factors that can play a role in the development of Morton's Neuroma. These include wearing ill fitting shoes that cause pressure
to the toes, such as high-heels. Also, high impact exercise may contribute to the cause of this condition. Morton’s Neuroma may also develop if
the foot sustains an injury. Another cause includes walking abnormally due to bunions or flat feet, which causes excessive pressure and irritates
the tissue. At times, people are affected for no apparent reason.
Podiatrists can alleviate the effects of this condition using a treatment plan to help decrease the pain, and heal the foot tissue. Depending upon
the severity of the Morton's Neuroma, the treatment plan can vary. For cases that are mild to moderate, treatments may include applying
padding to the arch to relieve pressure from the nerve and reduce compression while walking. Ice packs can also help reduce swelling, and the
podiatrist may devise a custom orthotic device to support the foot and reduce compression and pressure on the affected nerve. The doctor will
probably advise against partaking in activities that cause constant pressure on the affected area, and may provide wider shoes to ease the
pressure from the toes. If these treatments do not relieve the symptoms of this condition, the doctor may use injection therapy.
Surgical treatment may be recommended by the podiatrist if all other treatments fail to provide relief. Normally, the podiatric surgeon will
decide on either a surgical procedure that involves removal of the affected nerve or will choose surgery to release the nerve. After examination,
the surgeon will decide on the best approach to treat the problem.

Plantar Fasciitis
The plantar fascia is a connective tissue in the heel that stretches the bottom length of your foot. Plantar fasciitis is the inflammation of this
connective band, causing heel pain and overall discomfort while walking or standing. Although the condition is completely treatable, traditional
methods can take up to a year to start being effective.
Plantar fasciitis is caused by a number of everyday activities, so understanding and assessing the condition is paramount to managing and
treating it. One of the most common causes of plantar fasciitis is excessive running, especially with improper fitting or non-supportive shoes. By
over exercising and running, the plantar fascia gets overworked and overstretched, eventually causing tears in the tissue and inflammation. Along
with improper fitting shoes, over-pronation is a common cause of plantar fasciitis. By not having the right shoes to correct this issue, once again
the plantar fascia becomes overstretched and starts to tear, causing the inflammation.
Despite the common causes of plantar fasciitis, there are many different treatment options. For less severe cases, conservative home remedies
such as taking anti-inflammatory drugs to alleviate pain, applying ice packs to the bottom of your foot and heel, slowly stretching and exercising
your feet to re-strengthen the tissue, and using orthotic devices to overcome issues such as over-pronation are all ways to help manage your
plantar fasciitis.
For more severe cases however, there are still things that can be done. Shockwave therapy has become a common solution for plantar fasciitis
because it effectively breaks up the tissue on the bottom of your foot via sound waves which facilitates healing and regeneration, allowing you to
overcome the chronic pain caused by plantar fasciitis. Even if this doesn’t work, surgery is always a final option. Surgery on the tissue itself can be
done to permanently correct the issue and stop the inflammation and pain is your heels.
No matter what the case may be however, seeking the immediate care of your podiatrist is the first and best step to recovery. Even the slightest
amount of heel pain could be the first stages of plantar fasciitis and the initial onset of tearing and overstretching of that band of tissue. On top of
this, because the tearing of this tissue can be compounded if it remains ignored, it could become a more severe case than it needs to be. The
solution to this is early detection and early treatment, so be sure to talk to your podiatrist about the possibilities of plantar fasciitis if you’re
experiencing heel pain.

Sports Medicine
Foot and ankle injuries are common among people who participate in sports. Several factors contribute to this. They include failing to stretch or
warm up properly, not wearing the proper type of shoe and not taping or providing other types of support for the ankle or foot. The most
common foot and ankle injuries suffered by people involved in sport are plantar fasciitis, ankle sprains and Achilles tendon damage or ruptures.
If not treated properly they can lead to permanent disability.
Plantar fasciitis is a painful condition. It is inflammation of the plantar fascia, the thick fibrous band of tissue running from the heel to the base of
the toes. There are several effective treatments for this ailment. Doctors often proscribe rest, massages, stretching, night splints, physical therapy,
anti-inflammatory medication, corticosteroids or surgery usually in that order. The most effective treatment for plantar fasciitis is orthotics, such
as foot supports. Surgery is occasionally used as a last resort.
The Achilles tendon is the largest tendon in the body. It connects the calf muscles to the heel bone. Running, jumping and walking all impact this
tendon. Two common injuries to the Achilles tendon are tendinitis and a rupture of the tendon. Tendinitis is inflammation in the tendon often
caused by an increase in the amount and intensity of stress placed on it. It can either be treated non-surgically with rest, ice or anti-inflammatory
medication or surgery may be required. A rupture (tear) of the Achilles tendon can be treated by placing the lower leg in a cast for several weeks
or with surgery. Many physicians feel surgery is the better option because it lowers the risk of re-ruptures. Both methods require 4 to 6 months of
rehabilitation.
Ankle sprains are the most common sports related foot and ankle injury. A sprain occurs when the ligament holding the ankle bones and joint
stretches beyond its normal range. It can be treated non-surgically with a combination of rest, ice wrapped around the joint for 30 minutes
immediately after injury, compression by a bandage and elevating the ankle above the heart for 48 hours. This combination is referred to as
RICE. Severe ankle sprains in which the ligaments are torn may require arthroscopic or reconstructive surgery followed by rehabilitation.
Treating these injuries is relatively simple if they are identified and addressed early. Many athletes dismiss the initial aches and pains associated
with injury as just soreness or tired muscles. Their first response is usually to try to work through it. This can lead to serious problems. Many
minor injuries are made far more serious when athletes continue to put strain and pressure on them. That attitude can change a mild strain into
a serious strain and a minor tear into a rupture. Athletes should have unusual aches and pains evaluated by a skilled, licensed medical
professional.

Warts
Plantar warts are warts that are only found on the feet, hence the term “plantar”, which means “relating to the foot.” They are caused by the
human papillomavirus, or HPV, and occur when this virus gets into open wounds on the feet. The warts themselves are hard bumps on the foot
and easily recognizable, mostly found on the heels or ball of the foot. For the most part, plantar warts are non-malignant, but they can cause
some pain, discomfort, and are often unsightly, so removing them is often the first step taken.
Plantar warts can cause some pain while standing, sometimes felt as tenderness on the sole of your foot. Unless the wart has grown into the foot
behind a callus, you will be able to see the fleshy wart. Because plantar warts are not cancerous or dangerous, a podiatrist should only be
consulted if there is an excess amount of pain associated with having them, if they are affecting your walking, or if they continually come back.
However, anyone who suffers from diabetes or a compromised immune system disease should seek out care immediately.
Podiatrists are easily able to diagnose plantar warts. They usually scrape off a tiny bit of the rough skin in order to make tiny blood clots visible
and show the inside of these warts. However, a biopsy can be done if the doctor is not able to diagnose them from simply looking at them. For a
less invasive treatment option, topical creams can be used through a doctor’s prescription, which may help given enough time and patience.
Keep the wart covered for protection in between daily treatments.
The best way to avoid developing plantar warts is to avoid walking barefoot in public places, especially when you have open sores or cuts on your
feet. It is also important to avoid direct contact with any other warts you might have or warts other people might have, as they are highly
contagious.

Wound Care
Diabetics must be wary of all wounds, regardless of depth or size. Diabetes, a chronic disease in which the body cannot properly use glucose the
way it normally would, causes various complications that make wounds difficult to heal. Nerve damage or neuropathy will cause diabetics to
have trouble feeling the pain of a blister or cut until the condition has significantly worsened or become infected. A diabetic’s weakened immune
system can make even the most minor of wounds easily susceptible to infection. Diabetics are also more prone to developing narrow, clogged
arteries, and are therefore more likely to develop wounds.
Wounds should be taken care of immediately after discovery, as even the smallest of wounds can become infected if enough bacteria build up
within the wound. To remove dirt, wounds should be first rinsed under running water only. Soap, hydrogen peroxide, or iodine can irritate the
injury and should be avoided. To prevent infection, apply antibiotic ointment to the wound and cover it with a bandage. The bandage should be
changed daily. The skin around the wound may be cleaned with soap.
To prevent further exacerbation, see a doctor—especially if you have diabetes. Minor skin conditions can become larger problems if not properly
inspected. As the wound heals, make sure to avoid applying pressure to the affected area.
Learn about Wound Care at Illinois Foot & Ankle Center


Learn about Laser Therapy for Ankle Pain
Learn about Laser Therapy for Ankle Sprains
Learn about Laser Therapy for Arthritis
Learn about Laser Therapy for Fungal Toenails
Learn about Laser Therapy for Neuromas
Learn about Laser Therapy for Warts
If you are experiencing a medical emergency please dial
911 or visit the nearest urgent care or emergency
department.
Sitemap
Section 1557 Notice of Nondiscrimination
779-333-7419


Many people are surprised to learn the wide variety of services provided
by a podiatrist. Dr. May is trained and experienced in the latest
techniques and is prepared to provide you with the most comfortable
treatment possible.
Why Choose Illinois Foot & Ankle Center?
We put our patients first. Dr. May is committed to
understanding the needs of each patient and
explaining the treatment options available.

Our on-site digital x-ray means a diagnosis can
usually be made on your first visit, without extra
visits to the hospital or imaging center.

We offer the latest in cutting edge technology to
provide you with the best treatment options possible to
get you back on your feet sooner.

While the course of treatment may vary from patient to patient, many
of the conditions treated are very similar. There is, however, a very
wide variety of foot and ankle conditions that Dr. May is highly trained
to treat. Below are some of the more common ones and some
information on each of them.
Common Conditions Treated by Dr. May


2024 Illinois Foot &
Ankle Center, SC.
All rights reserved.
If you are experiencing a medical emergency please dial
911 or visit the nearest urgent care or emergency
department.
Sitemap
Section 1557 Notice of Nondiscrimination






















Achilles Tendon Disorders
The Achilles tendon is the strongest tendon in the human body. Its purpose is
to connect the lower leg muscles and calf to the heel of the foot. This tendon is
responsible for facilitating all types of movement, like walking and running.
Since this tendon provides an enormous amount of mobility to an individual,
any injuries inflicted to this tissue should be immediately brought up with a
physician to prevent further damage.
The most common injuries that can trouble the Achilles tendon are tendon
ruptures and Achilles tendinitis. Achilles tendinitis is the milder of the two
injuries and can be recognized by the following symptoms: inflammation, dull
to severe pain, an increased flow of blood to the tendon, thickening of the
tendon, and slower movement time. Tendinitis can be treated via several
methods and is often diagnosed by an MRI.
An Achilles tendon rupture is trickier to heal, and is by far the most painful
injury. It is caused by the tendon ripping or completely snapping. The results
are immediate and absolutely devastating, and will render the patient
immobile. If a rupture or tear occurs, operative and non-operative methods
are available. Once the treatment begins, depending on the severity of the
injury, recovery time for these types of issues can take up to a year.
Simple preventative measures can be taken as a means to avoid both injuries.
Prior to any movement, taking a few minutes to stretch out the tendon is a
great way to stimulate the tissue. Calf raises, squats, leg curls, leg extensions,
leg raises, lunges, and leg presses are all suggested ways to help strengthen
the lower legs and promote Achilles tendon health.
Many problems arise among athletes and people who overexert themselves
while exercising or who do not properly warm up before beginning an activity.
Proper, comfortable shoes that fit correctly can also decrease tendon injuries.
Some professionals also suggest that when exercising, you should make sure
that the floor you are on is cushioned or has a mat, as this will relieve pressure
on the heels. As always, a healthy diet will also increase tendon health.
It is very important to seek out a podiatrist if you believe you have an injury in
the Achilles region, because further damage could result in severe
complications that would make being mobile difficult, if not impossible.

Ankle Pain
Pain experienced in the ankle can be caused by a multitude of conditions.
While the most common cause is an ankle sprain, other possible problems can
include arthritis, gout, ankle instability, ankle fracture, nerve compression, or
tendinitis. In more serious cases, ankle pain can be a sign of improper
alignment of the foot or an infection.
Ankle pain can often be accompanied by symptoms such as redness, swelling,
stiffness and warm in the affected area. Pain can be described differently
depending on the condition; short, stabbing pain and a dull ache are some
examples. If such symptoms are persistent and do not improve after time, be
sure to schedule an appointment with your local podiatrist.
Depending on the condition behind your ankle pain, different treatments may
be prescribed by your podiatrist. For ankle sprains, the first step in treatment
involves rest, ice, elevation, and compression. Be sure to avoid placing
pressure on the ankle, use an ice pack several times a day, and use a
compression bandage and elevation to reduce swelling. Other more serious
conditions may require the assistance of certain drugs and medications such
as non-steroidal anti-inflammatory drugs (NSAIDs), physical therapy, or even
cortisone injections.
Consult with your foot and ankle doctor to best determine the cause of your
ankle pain and the appropriate treatment. Depending on the severity of your
ankle pain and the condition behind it, recovery from ankle pain may take
some time.

Ankle Sprains
Ankle sprains can be serious and should be given immediate attention and
care, despite not being as severe as a broken ankle. An ankle sprain can lead to
a significant amount of pain, as well as limited mobility. They are often
characterized by swelling and discoloration of the skin, which occurs when the
ligaments are stretched beyond their limits.
The simple act of walking can sometimes cause a sprain, which makes them a
very common injury for anyone. They occur when the ankle twists in an
awkward way or rolls over itself, causing a pop or snap in the tendons around
the ankle. Some people are more at risk than others, including athletes who
continually push their bodies to the limits and also people who have previously
suffered accidents to the feet, ankles, or lower legs.
If you believe you have an ankle sprain, it is important to consult with your
podiatrist right away. Ankle sprains can turn into severe injuries that may
require hospitalization. If the ankle ligaments or muscles are damaged from a
tear or rip, the sprain may be severe enough to warrant going to the hospital
and possibly having surgery done. Even after surgery the recovery process can
be long, often involving rehabilitation sessions with a podiatrist to get your
ankle back to full strength and health.
The severity of your sprain may become apparent if you are unable to stand or
walk, if non-stop pain is occurring over a prolonged period of time, if swelling
is much more severe than initially present, or if you start to experience
tingling or numbness. These signs may show that your ankle sprain might
actually be a broken ankle, which requires immediate medical attention.
While not completely avoidable, ankle sprains can be curbed with some
preventative treatment measures. These include wearing appropriate fitting
shoes that not only provide a comfortable fit, but also ankle support. It is also
recommended to stretch before doing any kind of physical activity, as this will
help lower your body’s chance for an injury.

Arthritic Foot and Ankle Care
During your lifetime, you will probably walk about 75,000 miles, which is
quite a lot of stress to put on your feet. As you get older, the 26 bones and 30
joints in your foot will lose flexibility and elasticity, and your foot’s natural
shock absorbers will wear down too. Having arthritis in addition to life’s wear
and tear only makes matters worse; the joints will become distorted and
inflamed, making arthritic foot care an important thing to consider for your
overall health.
When dealing with arthritis, having additional foot complications—such as
bunions, hammertoes, or neuromas—may be a serious detriment. To avoid
these, buying well-fitting shoes with a lower heel and good support is a must.
Having shoes with good arch support is highly recommended.
Aside from getting good arch support, the shoes need to fit comfortably and
properly as well. A good place to start is by leaving a finger width between the
back of the shoe and your foot to gauge proper size. It is also helpful to have a
square or rounded toe box in the front to provide even more comfort. Another
thing to look for is a rubber sole that can provide a cushion and absorb shock
as you walk. This adds flexibility to the ball of your foot when you push off
your heel to walk.
Exercise is another key aspect of arthritic foot care, as it not only strengthens
and stretches the muscles and joints but helps prevent further injury and pain
as well. Certain non-steroid, non-inflammatory drugs or topical medicines
may be recommended by your podiatrist to help ease arthritic pain. Be sure to
visit your podiatrist to determine what method of care is best for you.

Athlete’s Foot (Foot Fungus)
Athlete’s foot is an extremely contagious infection caused by a fungus that
results in itching, burning, dry, and flaking feet. The fungus that causes
Athlete’s foot is known as tinea pedis and thrives in moist, dark areas such as
shower floors, gyms, socks and shoes, commons areas, public changing areas,
bathrooms, dormitory style houses, locker rooms, and public swimming pools.
Athlete’s foot is difficult to treat as well because of the highly contagious and
recurrent nature of the fungus.
Athlete’s foot is spread by direct contact with an infected body part,
contaminated clothing, or by touching other objects and body parts that have
been exposed to the fungus. Because the feet are an ideal place for tinea to
grow, thrive, and spread, this is the most commonly affected area, but it is
known to grow in other areas.
The most commonly infected body parts are the hands, groin, and scalp, as
well as obviously the feet. Around 70% of the population suffer from tinea
infections at some point in their lives, however not all of these cases are
Athlete’s foot. Just like any other ailment, some people are more likely to get it
than others; such as people with a history of tinea infections or other skin
infections, both recurring and non-recurring ones. On top of this, the extent to
which a person experiences regrowth and recurrent tinea infections varies
from person to person.
Sometimes people will not even know that have Athlete’s foot because of a lack
of symptoms. However, most people experience mild to moderate flaking,
itching, redness, and burning. Some of the more severe symptoms include
cracking and bleeding skin, intense itching and burning, pain while walking or
standing, and even blistering.
Because of the recurring nature of tinea fungus and the Athlete’s foot it causes,
the best way to treat this condition is with prevention. While it is hard to
completely avoid, you can take some preventative measures such as wearing
flip flops or sandals in locker rooms and public showers to reduce contact with
the floor. It is important to keep the feet clean and dry, which will allow them
to air out and breathe. If you suspect you have Athlete’s foot, immediately visit
your local podiatrist to determine what treatment is best for you.

Bunions
A bunion is an enlargement of boney growth or swollen tissue typically located at the base
joint of the big toe. The condition is caused by the shifting of the bones in the big toe
inward, toward the other toes of the foot. The area around the base of the big toe may
become inflamed, red, and painful.
Genetic factors are important in the formation of bunions – people who get bunions are
usually genetically predisposed to this bone displacement and may cause its onset by
wearing ill-fitting shoes or by running or walking in a way that causes stress to the feet.
Another common cause for bunions is wearing high heeled shoes. The weight of the body
in these shoes pushes the toes into an unnatural position, possibly causing bone
displacement.
A podiatrist who specializes in foot structure and biomechanics can quickly diagnose
bunions. Bunions must be distinguished from gout or arthritic conditions, so blood tests
may be necessary. The podiatrist may order a radiological exam to provide an image of the
bone structure. If the x-ray demonstrates an enlargement of the joint near the base of the
toe and a shifting toward the smaller toes, this is indicative of a bunion.
Wearing wider shoes can remove the pressure on the bunion and reduce pain. High heeled
shoes should be eliminated for a period of time as this type of shoe generally pushes the
big toe outward toward the smaller toes. This may be enough to eliminate the pain
associated with bunions; however, if pain persists, anti-inflammatory drugs may be
prescribed. Severe pain may require an injection of steroids near the bunion.
Orthotics for shoes may be prescribed which, by altering the pressure on the foot, can be
helpful in reducing pain. These do not correct the problem, but by eliminating the pain,
they can provide relief.
For cases that do not respond to these methods of treatment, surgery can be done to
reposition the toe. A surgeon may do this by either taking out a section of bone or by
rearranging the ligaments and tendons in the toe to help keep it properly aligned. It may
be necessary even after surgery to wear more comfortable shoes that do not put pressure
on the toe as the big toe can easily move back to its orientation toward the smaller toes.

Corns
Corns are thickened areas on the skin’s surface, to the point of being irritating and
sometimes painful. Commonly found on the feet, corns are circular or cone-shaped and
develop where there are areas of pressure or friction, such as on the little toe when it rubs
up against shoes or on the ball of your foot.
Corns are often confused with a callus, but there is a difference between them. Corns can
be raised bumps that are painful to the touch. They consist of a rough, thick area of skin
that may be dry or waxy. Corns tend to be surrounded by skin that is inflamed, and are
usually much smaller than calluses.
The best treatment for a corn varies from person to person and is best determined by a
podiatrist. Certain topical over-the-counter products may be suggested, or a more serious
treatment may be prescribed. Diabetics should consult with a podiatrist immediately if
they have developed a corn, as small wounds such as corns can develop into more serious
conditions.
Orthotic inserts, which are fitted by a podiatrist, may also help with treating corns. Inserts
fit right into the shoes and adjust the way the feet fit into the shoes, thus fixing the way one
walks. Proper-fitting orthotics can help reduce friction, which can in turn help reduce corn
formation and exacerbation.
Surgery can be used to treat corns. Corn surgery actually deals with the underlying issue
that causes corns. During surgery, the bone is shaved and any abnormalities are corrected,
thus reducing the amount of friction that occurs during walking.
To prevent corns, the first step is reducing friction. Always wear shoes that fit well and
don’t rub the feet. Wearing cushioned insoles in your shoes can also reduce friction. While
there are many ways to prevent corns, it is best to consult a podiatrist with any questions
you may have.

Custom Orthotics
Orthotics are shoe inserts that are meant to correct an irregular walking gait or provide
cushioning to the feet. Orthotics come in a variety of different models and sizes, including
over-the-counter and customizable variants. Customizable orthotics can be shaped and
contoured to fit inside a specific shoe and are typically prescribed through a podiatrist
who specializes in customized footwear and orthotics design and management.
Customized footwear and orthotics design and management. Orthotics are beneficial
because they can help prevent injuries from occurring and provide cushioning to keep
pain levels down to a minimum. They also allow for the correct positioning of the feet.
Orthotics can act as shock absorbers to help remove pressure from the foot and ankle.
Therefore, orthotics can make bodily movements, such as walking and running, become
more comfortable as well as help prevent the development of certain foot conditions.
Orthotics alleviate pain and make the foot more comfortable by slightly altering the angle
at which the foot strikes the ground surface, therefore controlling the movement of the
foot and ankle. Orthotics come in different variants and can be made of various materials.
To determine what type of orthotic is most suited to your feet and your needs, it is best to
consult your podiatrist. He or she will be able to recommend a type of orthotic that can
help improve your foot function or prescribe a custom orthotic to best fit your feet.

Diabetic Foot Care
Diabetes affects millions of people every year. Blood vessels located all over the body are
damaged due to diabetes—even the blood vessels of the feet. Neuropathy, or nerve
damage, can result from slower blood flow in the legs and feet. In diabetic patients
neuropathy is very important to monitor, as diabetics are at risk for developing ulcers.
Always washing and thoroughly drying the feet are pertinent parts of diabetic foot care.
There should be a focus on cleaning between the toes. Even if no pain is felt, the entire
foot should be examined for redness and sores. Neuropathy can often mask the pain of
sores and ulcers, and cause these conditions to be overlooked. Use a mirror to examine the
underside of your feet if needed. It is recommended that diabetics wear will-fitting socks.
Patients with diabetes should have their doctor monitor their blood levels because blood
sugar levels play a huge role in diabetic care. Monitoring these levels on a regular basis is
highly advised. It is very important to keep your blood sugar levels in the normal range,
which can be determined by your physician. There are medications that a physician may
prescribe to help with neuropathy of the diabetic patient. It is also advisable to visit a
podiatrist if the diabetic patient is experiencing any conditions involving the feet such as
ingrown toenails, which in more severe cases can cause infection.
Diabetic foot care at home is possible if a patient is provided with instructions from their
physician. Patients can cure dry heels with creams or ointments. If trying to remove a
callus with a tool, practice caution as severe diabetics may not be able to feel pain.
Improper removal may cause a wound to develop.
Diabetic feet must be inspected on a daily basis. Set up regular visits with your podiatrist
since proper diabetic foot care is necessary. If you suspect that you have a wound, notify
your doctor immediately. Gangrene is a serious problem for diabetics and can lead to
sepsis and amputation in its worst cases. Early treatment and daily inspection of diabetic
feet are keys to staying healthy.
Learn about Diabetic Foot Care

Flat Feet
Flat feet is a condition in which the arch of the foot is depressed, generally making the sole
of the foot completely or almost completely stay in contact with the ground. About 20-
30% of the population generally has flat feet because their arch never formed during
growth.
Having flat feet can sometimes make it difficult to walk due to the stress it places on the
ankles. The general alignment of your legs is thrown off because the ankles move more
inward which can cause some major discomfort. This also has a big effect on the knees as
many people that have flat feet often have arthritis in that area. However, in many cases,
having flat feet do not cause any pain and it should not be a cause for concern in that case.
For those who run, there are specific shoes to help realign the ankles with a lot more
support and less pronation. The weight shifting in this activity is very quick, so that's why
it's important to know if you have flat feet early on in your life, in case of injury down the
road.
Symptoms of flat feet can include: pain around the heel or arch area, trouble standing on
the tip toe, swelling around the inside of the ankle, flat look to one or both feet, and having
your shoes feel uneven when worn. A major cause of flat feet is never having developed an
arch on your foot. Overtime, a lot of stress and trauma to the foot can actually weaken the
posterior tibial tendon that runs around the inside of the ankle. This is the reason why
some people with flat feet have pain around that particular area.
There are a number of ways to help treat flat feet. One way is going barefoot. Studies have
shown that those that grew up going barefoot or wearing less closed-toe shoes actually
have more of an arch because the general strength and fullness of the arch increased. Also,
those with flat feet have a weaker Achilles tendon, and exercise to the area will help stretch
the area. In a lot of cases, there are great shoe inserts provided by podiatrists to provide
ankle support as well as reduce the symptoms that go along with severe flat feet. For those
that suffer severe pain in that area, tendon surgery is an option to help with any posterior
tibial tears.

Foot Pain
The feet, being the foundation of the body, carry all of the body’s weight and are therefore
prone to experiencing pain and discomfort. If you are experiencing foot pain, it is
important to determine where in the foot you are experiencing this pain to help discover
the cause of it. While pain can be experienced virtually anywhere in the foot, the most
common sites of foot pain are in the heel and ankle.
Heel pain can be due to a multitude of conditions including plantar fasciitis, Achilles
tendinitis, and heel spurs. Pain experienced in the ankle can be a sign of an ankle sprain,
arthritis, gout, ankle instability, ankle fracture, or nerve compression. In more serious
cases, pain the foot can be a sign of improper alignment or an infection.
Foot pain can be accompanied by symptoms including redness, swelling, stiffness and
warmth in the affected area. Whether the pain can be described as sharp or dull depends
on the foot condition behind it. It is important to visit your local podiatrist if your foot
pain and its accompanying symptoms persist and do not improve over time.
Depending on the location and condition of your foot pain, your podiatrist may prescribe
certain treatments. These treatments can include but are not limited to prescription or
over-the-counter drugs and medications, certain medications, laser treatment, shockwave
therapy, cortisone injections, or surgery.
If you are experiencing persistent foot pain, it is important to consult with your foot and
ankle doctor to determine the cause and location. He or she will then prescribe the best
treatment for you. While milder cases of foot pain may respond well to rest and at-home
treatments, more serious cases may take some time to fully recover.

Foot Surgery
In most cases, foot surgery is often chosen as the last-available option for conditions that
have otherwise been unsuccessfully treated. Surgery may be necessary for several reasons,
including the removal of foot deformities (e.g. bone spurs or bunions), arthritis problems,
reconstruction due to injury, and congenital malformations (e.g. club foot or flat feet).
Regardless of one’s age, foot surgery may be the only successful option for treatment for
certain conditions.
The type of surgery one undergoes depends on the type of foot condition the patient has.
For the removal of a growth, such as a bunion, a bunionectomy is necessary. If the bones in
the feet need to be realigned or fused together, a surgical fusion of the foot is needed. For
pain or nerve issues, a patient may require surgery in which the tissues surrounding the
painful nerve are removed. Initially, less invasive treatments are generally attempted;
surgery is often the last measure taken if other treatments are unsuccessful.
While in many cases surgery is often deemed as the final resort, choosing surgery comes
with certain benefits. The associated pain experienced in relation to the particular
condition is often relieved with surgery, allowing patients to resume daily activities. The
greatest benefit, however, is that surgery generally eliminates the problem immediately.
Podiatry history has shown that foot treatments continue to evolve over time. As
technology vastly improves, so will the various techniques in foot surgery, which already
require smaller and smaller incisions with the use of better and more efficient tools.
Thanks to such innovations, surgery is no longer as invasive as it was in the past, allowing
for much faster and easier recoveries.

Fungal Toenails
Toenail fungus is a condition that many people develop and suffer from. Toenail fungus
often results in the discoloration and thickening of the toenail, which can cause
embarrassment for many people. The condition begins as a small white or yellow growth
beneath the tip of the nail and at its worse can develop into the nail’s deterioration.
Thick, ragged, and distorted nails lacking shine are a sign of toenail fungus. The color of
the affected nail tends to be darker because of debris buildup underneath the nail. Toenail
fungus is more likely to develop for people who wear socks and shoes that do not allow
decent ventilation of the feet. Public showers, gyms, and swimming pools are breeding
grounds for toenail fungus, as their damp and humid environments allow for the growth
of bacteria.
Patients should visit their local podiatrist if they suspect they have toenail fungus because
in its more severe stages, toenail fungus can become very painful. Other infections can
develop from toenail fungus that can spread to other parts of the body. Upon examination
for fungus, your podiatrist may scrape your nails if he or she finds debris. This will be sent
to a lab to determine what fungus is causing the condition.
Toenail fungus can also be treated with certain over-the-counter antifungal creams and
ointments. To remove pressure from the nails, keep them cut at a short length. Oral
antifungal drugs, medicated nail cream, or medicated nail polish may also be prescribed
by your podiatrist if simpler treatments do not prove successful. In some cases, your
podiatrist may also recommend laser treatment to eradicate toenail fungus.

Geriatric Foot
Care
While proper foot care is important for everybody, senior citizens have the tendency to be
more susceptible to certain conditions and should therefore be well informed about
problems that may arise and what they can do to properly avoid or treat them.
Some of the most common problems are foot ulcers, ingrown toenails, fallen arches, and
fungal infection. A foot ulcer is an open sore on the foot and can be a result of decreased
sensation in the feet. An ingrown toenail is defined as when the nail grows into the side of
the toe. Fallen arches are indicated by the instep of the foot collapsing. A fungal infection is
a condition that results in deformed and discolored toenails.
In order to avoid these conditions it is recommended that the feet be inspected by the
patient on a regular basis. If these inspections are carried out routinely, there is a good
likelihood that problems can be identified before they become severe, or can even be
avoided altogether. If any abnormality is discovered, it is important that the individual
consult a doctor for diagnosis and information on treatment options.
Proper foot hygiene is also important. Making sure that you always have clean, dry socks on
can be a major deterrent to many different problems including bacterial infections, foot
odor, and certain types of fungus. Wet feet are a major cause of many of these problems. If
your socks get wet, it is important to change them. Walking around in wet socks may not
only lead to various infections, but can irritate the skin and result in a number of various
complications. Clean, dry feet are less likely to be affected by fungal and other infections.
As people age, the fat present on your feet begins to deteriorate. The protective nature of
this fat keeps the feet healthy by providing a barrier and between your bones and the
ground as well as giving the skin on the foot a certain amount of elasticity. This is one
factor that causes elderly people to develop some serious foot issues. Foot moisturizers can
be helpful to avoid certain problems associated with this.
However, water-based moisturizers do not work as well for elderly people as they do for the
young. Instead, it is more effective to use an emollient instead. An emollient is effective
because it binds the water in the foot, keeping it from becoming absorbed too readily which
will result in dry skin. They also have a special property called occlusion, which provides a
layer of oil on the skin. This layer prevents the foot from drying up and can be very effective
in treating dry skin disorders. If you can keep the skin on your feet healthy, this will
substantially reduce the number of foot problems you will encounter in old age.
Proper footwear is another way to keep feet healthy. Shoes that fit well and provide proper
support help prevent ingrown toenails and fallen arches.
Certain medical conditions such as diabetes or poor blood circulation increase the risk for
foot issues. For individuals with any of these conditions it is extremely important to
conduct regular foot inspections to make sure that there are no sores or infections present.

Hammertoe
Hammertoes are painful deformities that frequently form on the second, third, or fourth
toe. The condition is often caused by an issue in foot mechanics: the person’s particular gait
or the manner in which they walk, or shoes that do not comfortably fit the deformity.
Hammertoes can be formed after wearing shoes that are too narrow or short for the foot or
have excessively high heels. Shoes that are not properly sized will force the toes into a bent
position for long periods of time, causing the muscles to shorten and toes to bend into the
deformity of a hammertoe.
Hammertoe can also be caused by complications from rheumatoid arthritis, osteoarthritis,
trauma to the foot, heredity, or a cerebral vascular accident. Pain and difficult mobility of
the toes, deformities, calluses, and corns are all symptoms of a hammertoe.
Someone who suspects they have the symptoms of a hammertoe should consult with a
physician—particularly a podiatrist. Podiatrists diagnose and treat complications of the foot
and ankle. If the podiatrist discovers that the affected toes are still flexible, treatment for
the hammertoe may simply involve exercise, physical therapy, and better-fitting shoes.
Treatment for hammertoes typically involves controlling foot mechanics, such as walking,
through the use of customized orthotics.
For more serious cases in which the toes have become inflexible and rigid, surgery may be
suggested. During the operation, the toe would receive an incision to relieve pressure on the
tendons. A re-alignment of the tendons may then be performed by removing small pieces of
bone to straighten the toe. In some cases, the insertion of pins is needed to keep the bones
in the proper position as the toe heals. The patient is usually allowed to return home on the
same day as the surgery.
If surgery is performed to repair a hammertoe, following the postoperative directions of
your doctor is pertinent. Directions may include several stretches, picking up marbles with
your toes, or attempting to crumple a towel placed flat against your feet. Wear shoes that
have low heels and a wide amount of toe space to maintain comfort. Closed shoes and high
heels should be avoided. Shoes with laces allow the wearer to adjust how fitted her or she
may want the shoes to be and also allow for greater comfort. To provide adequate space for
your toes, select shoes that have a minimum of one-half-inch of space between the tip of
your longest toe and the inside of the shoe. This will also relieve pressure on your toes and
prevent future hammertoes from forming. Other preventative measures that can be taken
include going shopping for new shoes in the middle of the day. Your feet are its smallest in
the morning and swell as the day progresses; trying on and purchasing new shoes midday
will give you the most reliable size. Be sure to check that the shoes you purchase are both
the same size. If possible, ask the store to stretch out the shoes at its painful points to allow
for optimum comfort.

Heel Pain
Have you ever gotten up from a chair or out of bed in the morning, and upon taking that
first step, feel like your heel has stepped on a tack? Many people experience a feeling of
sharp pain which radiates into their arch from their heel and which does not allow them to
put their heel on the floor. Sometimes they need to sit back down, stand only on their toes
and use the wall for balance. If you can take a few steps, it seems to go away and lessens,
allowing you then to resume your activity. Later, throughout your day and after a period of
rest, it can happen again. If this sounds familiar you may be suffering from your first attack
of heel pain.
Heel pain is a debilitating condition that affects day to day activities. Running and walking
both cause stress on the heel because the heel is the part of the foot that hits the ground
first. This means that the heel is taking on your entire weight. Diagnosis and treatments for
heel pain can be easily found through your podiatrist.
Plantar Fasciitis
One of the main causes of heel pain is a condition known as plantar fasciitis. The plantar
fascia is a band of tissue that extends along the bottom of the foot, from the toe to the
bottom of the heel. A rip or tear in this ligament can cause inflammation of these tissues,
resulting in heel pain. People who do not wear proper fitting shoes are often at risk of
developing problems such as plantar fasciitis. Unnecessary stress from ill-fitting shoes,
weight change, excessive running, and wearing non-supportive shoes on hard surfaces are
all causes of plantar fasciitis.
Achilles Tendinitis
Achilles tendinitis is another cause of heel pain. Similar to plantar fasciitis, inflammation of
the Achilles tendon will cause heel pain due to stress fractures and muscle tearing. A lack of
flexibility of the ankle and heel is an indicator of Achilles tendinitis. If left untreated, this
condition can lead to plantar fasciitis and cause even more pain on your heel.
Heel Spur
A third cause of heel pain is a heel spur. A heel spur occurs when the tissues of the plantar
fascia undergo a great deal of stress, leading to a separation of the ligament from the heel
bone entirely. This results in a pointed fragment of bone on the ball of the foot, known as a
heel spur.

Heel Spurs
Heel spurs are essentially a hook of bone that forms at the back of the foot, at the base of
the ankle. Heel spurs are also described as a calcium deposit that covers the tendons and
ligaments of the ankle. Heel spurs cause extreme pain, and can prevent someone from
walking or being physically active at a normal level.
Heel spurs are more common than people expect them to be. They are most common in
people age forty and over, although heel spurs can occur in people younger than forty, and
frequently affect athletes or people who are very physically active. Heel spurs are also
common in those with poor circulation and degenerative diseases. People who suffer from
arthritis may suffer from heel spurs as well.
The symptoms of heel spurs are pain in the lower ankle, which increase when walking.
Treatment of heel spurs can be treated many ways and most often times is very effective. If
someone suspects that they have heel spurs, they should contact their physician. Their
physician will recommend that they perform an x-ray on the patient's ankles. The physician
may also perform a physical on the patient to ensure that there are no underlying
conditions, and of course if heel spurs are discovered a physician can recommend
treatment options.
Orthopedic shoes are specially designed footwear for people who suffer with foot problems.
Orthopedics offer a rubber sole, which cushions the heel and adds comfort to those who
suffer from heel spurs. Another simple way to help the pain of heel spurs is to elevate the
ankle to diminish the pain. When elevating the ankle, the blood is not focused on that area
of the foot and can bring some relief. When all these options have been attempted, and
there is still no relief from heel spurs, or the heel spurs return, surgery can be the more
dramatic and permanent way to rid patient of heel spurs.
There are less conventional ways that are becoming more popular ways to treat heel spurs.
One option would be to use a night splint which reduces the pain caused from heel spurs if
worn overnight. Other alternative treatment methods that can be used are ultrasound, or
acupressure. There are also other tolls that can be used are heel cups, heel seats, heel pads,
arch supports, and insoles.
Exercise is also another powerful tool to help alleviate pain from heel spurs and can help in
dealing with some of the symptoms, although exercising incorrectly and forgetting to
protect your feet can lead to further pain. It is important to remember the correct way to
place the feet when exercising so as to avoid making the problems worse, or creating
problems. When exercising to alleviate heel spurs, exercising strengthens muscles around
the surrounding tissue around the ankle. Stretching will also keep the tendons around the
ankle flexible.

Ingrown Toenails
An ingrown toenail is caused when a toenail grows sideways into the bed of the nail,
causing pain and swelling. The nail can sometimes exacerbate and become infected,
creating serious drainage.
There are many risk factors that can predispose a person to this common condition.
Cutting your nails too short, participating in sports, diabetes, being overweight, or having
a fungal infection of the toe can all cause an ingrown toenail. The condition can often be
related to genetics, as many people are genetically predisposed to ingrown nails. More
often than not, the problem can arise from wearing ill-fitting shoes or from shoes that
keep the feet slightly damp.
To prevent ingrown toenails, allow your toenails to grow a little longer and avoid cutting
them too short. If you do develop an ingrown nail, soaking the toe in hot water will help
prevent infection and lessen pain. You may want to add antibiotic soap or Epsom salts to
the water, which will provide further protection against infection.
There are many quick treatments available for ingrown toenails that can lessen pain and
have you walking with comfort. If your pain is so severe that it keeps you from everyday
activities, however, a visit with your podiatrist is necessary.

Neuromas


Plantar Fasciitis
The plantar fascia is a connective tissue in the heel that stretches the bottom length of your
foot. Plantar fasciitis is the inflammation of this connective band, causing heel pain and
overall discomfort while walking or standing. Although the condition is completely
treatable, traditional methods can take up to a year to start being effective.
Plantar fasciitis is caused by a number of everyday activities, so understanding and
assessing the condition is paramount to managing and treating it. One of the most common
causes of plantar fasciitis is excessive running, especially with improper fitting or non-
supportive shoes. By over exercising and running, the plantar fascia gets overworked and
overstretched, eventually causing tears in the tissue and inflammation. Along with
improper fitting shoes, over-pronation is a common cause of plantar fasciitis. By not having
the right shoes to correct this issue, once again the plantar fascia becomes overstretched
and starts to tear, causing the inflammation.
Despite the common causes of plantar fasciitis, there are many different treatment options.
For less severe cases, conservative home remedies such as taking anti-inflammatory drugs
to alleviate pain, applying ice packs to the bottom of your foot and heel, slowly stretching
and exercising your feet to re-strengthen the tissue, and using orthotic devices to overcome
issues such as over-pronation are all ways to help manage your plantar fasciitis.
For more severe cases however, there are still things that can be done. Shockwave therapy
has become a common solution for plantar fasciitis because it effectively breaks up the
tissue on the bottom of your foot via sound waves which facilitates healing and
regeneration, allowing you to overcome the chronic pain caused by plantar fasciitis. Even if
this doesn’t work, surgery is always a final option. Surgery on the tissue itself can be done to
permanently correct the issue and stop the inflammation and pain is your heels.
No matter what the case may be however, seeking the immediate care of your podiatrist is
the first and best step to recovery. Even the slightest amount of heel pain could be the first
stages of plantar fasciitis and the initial onset of tearing and overstretching of that band of
tissue. On top of this, because the tearing of this tissue can be compounded if it remains
ignored, it could become a more severe case than it needs to be. The solution to this is early
detection and early treatment, so be sure to talk to your podiatrist about the possibilities of
plantar fasciitis if you’re experiencing heel pain.

Sports Medicine
Foot and ankle injuries are common among people who participate in sports. Several
factors contribute to this. They include failing to stretch or warm up properly, not wearing
the proper type of shoe and not taping or providing other types of support for the ankle or
foot. The most common foot and ankle injuries suffered by people involved in sport are
plantar fasciitis, ankle sprains and Achilles tendon damage or ruptures. If not treated
properly they can lead to permanent disability.
Plantar fasciitis is a painful condition. It is inflammation of the plantar fascia, the thick
fibrous band of tissue running from the heel to the base of the toes. There are several
effective treatments for this ailment. Doctors often proscribe rest, massages, stretching,
night splints, physical therapy, anti-inflammatory medication, corticosteroids or surgery
usually in that order. The most effective treatment for plantar fasciitis is orthotics, such as
foot supports. Surgery is occasionally used as a last resort.
The Achilles tendon is the largest tendon in the body. It connects the calf muscles to the
heel bone. Running, jumping and walking all impact this tendon. Two common injuries to
the Achilles tendon are tendinitis and a rupture of the tendon. Tendinitis is inflammation in
the tendon often caused by an increase in the amount and intensity of stress placed on it. It
can either be treated non-surgically with rest, ice or anti-inflammatory medication or
surgery may be required. A rupture (tear) of the Achilles tendon can be treated by placing
the lower leg in a cast for several weeks or with surgery. Many physicians feel surgery is the
better option because it lowers the risk of re-ruptures. Both methods require 4 to 6 months
of rehabilitation.
Ankle sprains are the most common sports related foot and ankle injury. A sprain occurs
when the ligament holding the ankle bones and joint stretches beyond its normal range. It
can be treated non-surgically with a combination of rest, ice wrapped around the joint for
30 minutes immediately after injury, compression by a bandage and elevating the ankle
above the heart for 48 hours. This combination is referred to as RICE. Severe ankle sprains
in which the ligaments are torn may require arthroscopic or reconstructive surgery followed
by rehabilitation.
Treating these injuries is relatively simple if they are identified and addressed early. Many
athletes dismiss the initial aches and pains associated with injury as just soreness or tired
muscles. Their first response is usually to try to work through it. This can lead to serious
problems. Many minor injuries are made far more serious when athletes continue to put
strain and pressure on them. That attitude can change a mild strain into a serious strain
and a minor tear into a rupture. Athletes should have unusual aches and pains evaluated by
a skilled, licensed medical professional.

Warts
Plantar warts are warts that are only found on the feet, hence the term “plantar”, which
means “relating to the foot.” They are caused by the human papillomavirus, or HPV, and
occur when this virus gets into open wounds on the feet. The warts themselves are hard
bumps on the foot and easily recognizable, mostly found on the heels or ball of the foot. For
the most part, plantar warts are non-malignant, but they can cause some pain, discomfort,
and are often unsightly, so removing them is often the first step taken.
Plantar warts can cause some pain while standing, sometimes felt as tenderness on the sole
of your foot. Unless the wart has grown into the foot behind a callus, you will be able to see
the fleshy wart. Because plantar warts are not cancerous or dangerous, a podiatrist should
only be consulted if there is an excess amount of pain associated with having them, if they
are affecting your walking, or if they continually come back. However, anyone who suffers
from diabetes or a compromised immune system disease should seek out care immediately.
Podiatrists are easily able to diagnose plantar warts. They usually scrape off a tiny bit of the
rough skin in order to make tiny blood clots visible and show the inside of these warts.
However, a biopsy can be done if the doctor is not able to diagnose them from simply
looking at them. For a less invasive treatment option, topical creams can be used through a
doctor’s prescription, which may help given enough time and patience. Keep the wart
covered for protection in between daily treatments.
The best way to avoid developing plantar warts is to avoid walking barefoot in public
places, especially when you have open sores or cuts on your feet. It is also important to
avoid direct contact with any other warts you might have or warts other people might have,
as they are highly contagious.

Wound Care
Diabetics must be wary of all wounds, regardless of depth or size. Diabetes, a chronic
disease in which the body cannot properly use glucose the way it normally would, causes
various complications that make wounds difficult to heal. Nerve damage or neuropathy will
cause diabetics to have trouble feeling the pain of a blister or cut until the condition has
significantly worsened or become infected. A diabetic’s weakened immune system can
make even the most minor of wounds easily susceptible to infection. Diabetics are also
more prone to developing narrow, clogged arteries, and are therefore more likely to
develop wounds.
Wounds should be taken care of immediately after discovery, as even the smallest of
wounds can become infected if enough bacteria build up within the wound. To remove dirt,
wounds should be first rinsed under running water only. Soap, hydrogen peroxide, or
iodine can irritate the injury and should be avoided. To prevent infection, apply antibiotic
ointment to the wound and cover it with a bandage. The bandage should be changed daily.
The skin around the wound may be cleaned with soap.
To prevent further exacerbation, see a doctor—especially if you have diabetes. Minor skin
conditions can become larger problems if not properly inspected. As the wound heals,
make sure to avoid applying pressure to the affected area.
Learn about Wound Care at Illinois
Foot & Ankle Center


Learn about Laser Therapy for
Ankle Pain
Learn about Laser Therapy for
Ankle Sprains
Learn about Laser Therapy for
Arthritis
Learn about Laser Therapy for
Fungal Toenails
Learn about Laser Therapy for
Neuromas
Learn about Laser Therapy for Warts